Reproductive Endocrinology focuses on hormones and their role in reproductive health. It deals with fertility, menstrual disorders, and menopause.
Reproductive Endocrinology is a specialized field within medicine that addresses hormonal functioning related to reproduction. It encompasses the diagnosis and treatment of conditions affecting fertility, menstrual cycles, and menopausal transitions. Hormonal imbalances can lead to various reproductive issues, including polycystic ovary syndrome (PCOS) and endometriosis.
Specialists in this field use advanced techniques to manage and treat these conditions. They often work with patients facing challenges such as infertility and recurrent pregnancy loss. Understanding the hormonal interplay is crucial for developing effective treatments. Reproductive endocrinologists play a vital role in helping individuals achieve reproductive health and wellness. They provide personalized care tailored to each patient’s unique hormonal profile.
What Is Reproductive Endocrinology
Reproductive Endocrinology is a fascinating field of medicine that focuses on hormones and their role in fertility and reproduction. It combines elements of gynecology, obstetrics, and endocrinology. This specialty helps individuals and couples navigate the complexities of reproductive health.
What Is Reproductive Endocrinology?
Reproductive Endocrinology is a subspecialty of obstetrics and gynecology. It involves diagnosing and treating hormonal disorders that affect fertility and reproductive health. Specialists in this field are called reproductive endocrinologists. They are experts in managing issues like infertility, menstrual disorders, and menopause.
Common Conditions Treated By Reproductive Endocrinologists
- Infertility: Difficulty in getting pregnant after a year of trying.
- PCOS (Polycystic Ovary Syndrome): A hormonal disorder causing enlarged ovaries with small cysts.
- Endometriosis: Tissue similar to the lining inside the uterus grows outside it.
- Menstrual Disorders: Irregular, heavy, or painful periods.
- Menopause: The natural decline in reproductive hormones when a woman reaches her 40s or 50s.
Diagnostic Methods In Reproductive Endocrinology
Reproductive endocrinologists use various diagnostic methods to identify hormonal imbalances and reproductive issues. These methods include:
| Method | Description |
|---|---|
| Blood Tests | Measure hormone levels in the blood. |
| Ultrasound | Visualize the reproductive organs. |
| Hysterosalpingography | X-ray of the uterus and fallopian tubes. |
| Laparoscopy | Minimally invasive surgery to examine the pelvic organs. |
Treatment Options In Reproductive Endocrinology
Treatment in reproductive endocrinology is tailored to the individual’s needs. Common treatments include:
- Medications: Hormone treatments to regulate menstrual cycles and ovulation.
- Assisted Reproductive Technologies (ART): Procedures like IVF (In Vitro Fertilization).
- Surgery: Correct structural problems in the reproductive organs.
- Lifestyle Changes: Diet and exercise modifications to improve reproductive health.
Reproductive endocrinology provides hope and solutions for those facing reproductive challenges. By understanding and addressing hormonal issues, reproductive endocrinologists help many achieve their dream of starting a family.
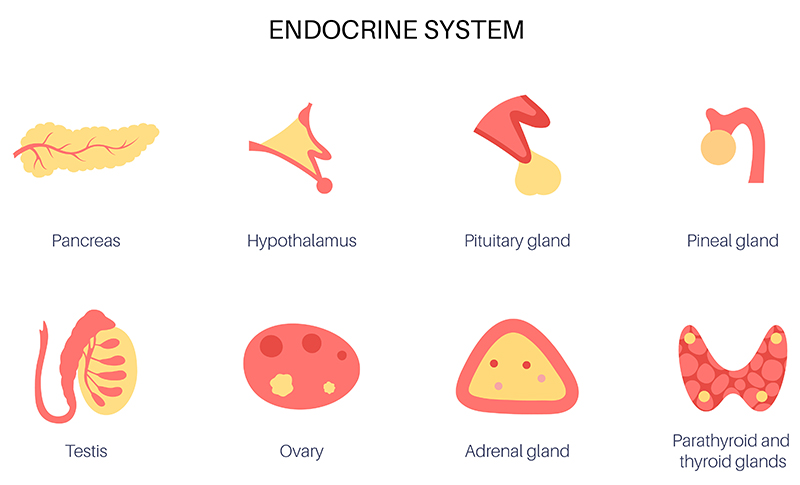
Credit: vetmed.tamu.edu
Key Hormones Involved
Reproductive endocrinology studies how hormones control reproductive functions. Key hormones like estrogen, progesterone, and testosterone play crucial roles in this complex system. Understanding these hormones helps in addressing various reproductive health issues.
Estrogen
Estrogen is vital for female reproductive health. It regulates the menstrual cycle, supports pregnancy, and affects various body systems.
Key functions of estrogen include:
- Regulating the menstrual cycle: Estrogen levels rise and fall during the cycle, influencing ovulation and menstruation.
- Supporting pregnancy: Estrogen prepares the uterus for pregnancy and supports fetal development.
- Bone health: Estrogen helps maintain bone density, reducing the risk of osteoporosis.
Estrogen levels vary by age and life stage. Here’s a quick look:
| Life Stage | Estrogen Level |
|---|---|
| Childhood | Low |
| Puberty | Rising |
| Reproductive Years | High |
| Menopause | Low |
High or low estrogen levels can cause health problems. High levels may lead to weight gain and menstrual issues. Low levels may cause hot flashes and mood swings.
Progesterone
Progesterone is another key hormone in reproductive health. It plays a vital role in the menstrual cycle and pregnancy.
Key functions of progesterone include:
- Preparing the uterus: Progesterone readies the uterine lining for a fertilized egg.
- Supporting pregnancy: It maintains the uterine lining and prevents contractions during pregnancy.
- Regulating the menstrual cycle: Progesterone levels drop if there is no pregnancy, leading to menstruation.
Progesterone levels fluctuate during the menstrual cycle:
| Phase | Progesterone Level |
|---|---|
| Follicular Phase | Low |
| Ovulation | Rising |
| Luteal Phase | High |
Low progesterone levels can lead to menstrual irregularities and difficulty in maintaining pregnancy. High levels are rare but may indicate certain health conditions.
Testosterone
Testosterone is often associated with male reproductive health but is also present in females. It impacts muscle mass, bone density, and sexual function.
Key functions of testosterone include:
- Development of male characteristics: Testosterone influences facial hair, voice deepening, and muscle growth.
- Maintaining libido: It plays a role in sexual desire and function in both males and females.
- Bone and muscle health: Testosterone supports bone density and muscle mass.
Testosterone levels vary by age and gender:
| Gender | Typical Range (ng/dL) |
|---|---|
| Male | 300-1,000 |
| Female | 15-70 |
Low testosterone levels in males can lead to fatigue, depression, and reduced libido. High levels in females may cause acne, hair loss, and irregular periods.
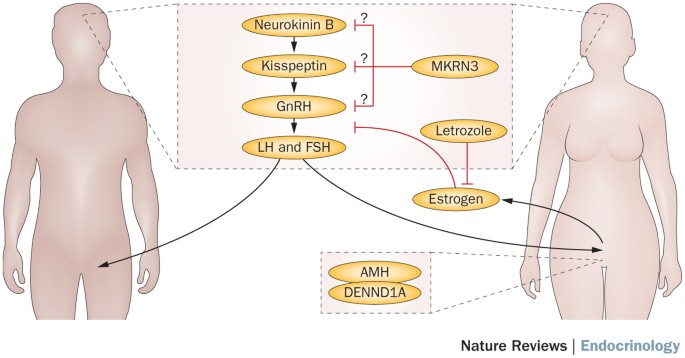
Credit: www.nature.com
Common Disorders
Reproductive Endocrinology deals with hormones and how they affect reproduction. Common disorders in this field can disrupt normal reproductive functions. These disorders can lead to symptoms like infertility, irregular periods, and hormonal imbalances. Understanding these conditions helps in managing and treating them effectively.
Polycystic Ovary Syndrome
Polycystic Ovary Syndrome (PCOS) is a hormonal disorder common among women of reproductive age. Women with PCOS may have infrequent or prolonged menstrual periods. They may also have excess male hormone (androgen) levels.
Key symptoms include:
- Irregular periods
- Excessive hair growth
- Weight gain
- Acne
PCOS can lead to infertility and metabolic problems. It is crucial to recognize the symptoms early for better management. Here is a table summarizing the main symptoms and their effects:
| Symptom | Effect |
|---|---|
| Irregular periods | Difficulty in conceiving |
| Excessive hair growth | Hirsutism |
| Weight gain | Increased risk of diabetes |
| Acne | Skin problems |
Early diagnosis and treatment are crucial. Lifestyle changes, medication, and hormonal therapy can help manage PCOS effectively.
Endometriosis
Endometriosis is a painful disorder. Tissue similar to the lining inside the uterus grows outside the uterus. This can cause severe pain and fertility issues.
Common symptoms include:
- Painful periods
- Pelvic pain
- Pain during intercourse
- Heavy menstrual bleeding
Endometriosis can also cause other complications like:
- Infertility
- Ovarian cysts
- Chronic fatigue
A proper diagnosis requires medical imaging and sometimes surgery. Here is a quick overview of the symptoms and their impact:
| Symptom | Impact |
|---|---|
| Painful periods | Debilitating pain |
| Pelvic pain | Chronic discomfort |
| Pain during intercourse | Relationship issues |
| Heavy menstrual bleeding | Anemia |
Endometriosis treatment includes pain relief, hormone therapy, and surgery. Early intervention helps manage the condition better.
Hypogonadism
Hypogonadism occurs when the body doesn’t produce enough sex hormones. It affects both men and women, leading to various symptoms and complications.
Symptoms in men include:
- Low libido
- Erectile dysfunction
- Reduced muscle mass
- Fatigue
Symptoms in women include:
- Irregular menstrual cycles
- Hot flashes
- Vaginal dryness
- Decreased libido
Here is a table summarizing the symptoms and their effects:
| Symptom | Effect |
|---|---|
| Low libido | Reduced sexual desire |
| Erectile dysfunction | Sexual difficulties |
| Reduced muscle mass | Weaker physique |
| Fatigue | Decreased energy |
| Irregular menstrual cycles | Fertility issues |
| Hot flashes | Discomfort |
| Vaginal dryness | Pain during intercourse |
Hypogonadism treatment includes hormone replacement therapy. Lifestyle changes and medication also help manage the symptoms effectively.
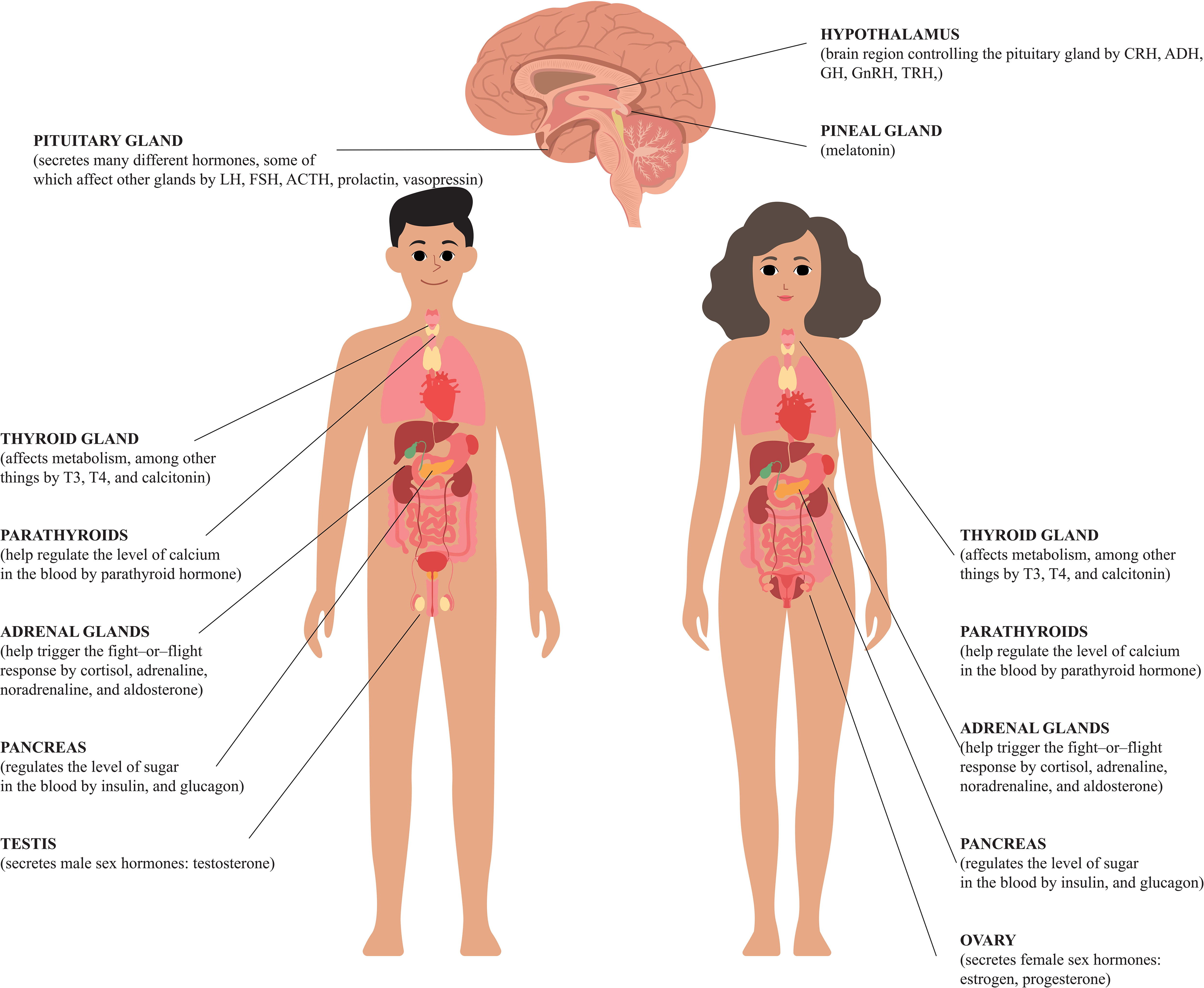
Credit: www.frontiersin.org
Diagnostic Procedures
Reproductive Endocrinology focuses on the hormonal functioning of the reproductive system. Diagnostic procedures play a crucial role in identifying and understanding various reproductive health issues. These procedures help in developing effective treatment plans. Some common diagnostic procedures include blood tests, imaging techniques, and biopsies.
Blood Tests
Blood tests are fundamental in diagnosing reproductive endocrine disorders. They help measure hormone levels, which provide insights into reproductive health. Common hormones tested include:
- Follicle-Stimulating Hormone (FSH)
- Luteinizing Hormone (LH)
- Estradiol
- Progesterone
- Testosterone
- Thyroid Stimulating Hormone (TSH)
- Prolactin
Blood tests can identify issues like polycystic ovary syndrome (PCOS), thyroid disorders, and pituitary gland problems. They are usually conducted at specific times in the menstrual cycle for accurate results. For example, FSH and LH are best tested on the third day of the cycle.
The results help doctors understand ovarian reserve, menstrual cycle irregularities, and other hormonal imbalances. Blood tests are usually quick, involving a simple blood draw, and results are often available within a few days.
Imaging Techniques
Imaging techniques provide visual insights into the reproductive organs. These techniques help in diagnosing structural abnormalities, cysts, and other issues. Common imaging techniques include:
- Ultrasound: Uses sound waves to create images of the ovaries, uterus, and fallopian tubes.
- Hysterosalpingography (HSG): An X-ray technique that examines the uterus and fallopian tubes using a contrast dye.
- Magnetic Resonance Imaging (MRI): Provides detailed images of reproductive organs using magnetic fields and radio waves.
- Sonohysterography: Combines ultrasound with saline solution to get a clearer view of the uterine cavity.
Ultrasound is the most commonly used imaging technique. It helps in tracking follicle development and identifying cysts or fibroids. HSG is particularly useful for checking fallopian tube blockages, which can affect fertility.
Doctors use imaging results to diagnose conditions like endometriosis, fibroids, and congenital anomalies. These techniques are non-invasive and usually painless, making them a preferred choice for initial diagnosis.
Biopsy
A biopsy involves taking a small tissue sample for examination under a microscope. It helps diagnose various conditions by providing detailed information about cellular structures. Common types of biopsies in reproductive endocrinology include:
- Endometrial Biopsy: Examines the lining of the uterus to diagnose abnormalities.
- Ovarian Biopsy: Checks for ovarian tumors or cysts.
- Cervical Biopsy: Diagnoses cervical dysplasia or cancer.
Endometrial biopsy is often used to investigate causes of abnormal uterine bleeding or infertility. It helps in diagnosing conditions like endometrial hyperplasia or cancer. The procedure is usually quick and can be done in a doctor’s office.
Ovarian biopsy is less common but may be necessary if imaging tests reveal suspicious masses. Cervical biopsy is typically performed if a Pap smear indicates abnormal cells.
Biopsy results provide crucial information for developing a treatment plan. Though the procedure may cause slight discomfort, it is highly valuable for accurate diagnosis.
Treatment Options
Reproductive Endocrinology focuses on diagnosing and treating issues related to hormones and fertility. Various treatment options exist to help individuals achieve their reproductive goals. These treatments range from medication to lifestyle adjustments. Let’s explore some common treatment options.
Hormone Therapy
Hormone therapy involves using medications to balance or supplement hormones in the body. This treatment can address issues like irregular menstrual cycles, polycystic ovary syndrome (PCOS), and infertility. Hormone therapy can be administered in different forms:
- Oral pills
- Patches
- Injections
- Topical creams
Benefits of hormone therapy include regulating menstrual cycles, improving ovulation, and enhancing fertility. Doctors often monitor hormone levels through blood tests to adjust dosages. Common hormones used in therapy are:
| Hormone | Purpose |
|---|---|
| Estrogen | Regulate menstrual cycle |
| Progesterone | Support pregnancy |
| FSH (Follicle Stimulating Hormone) | Stimulate egg production |
| LH (Luteinizing Hormone) | Trigger ovulation |
Patients may experience side effects like mood swings, nausea, and headaches. Always consult a healthcare provider before starting hormone therapy.
Surgery
Surgical options can address structural problems in the reproductive system. Common procedures include:
- Laparoscopy: Minimally invasive surgery to diagnose and treat conditions like endometriosis and ovarian cysts.
- Hysteroscopy: A procedure to examine and treat abnormalities inside the uterus.
- Myomectomy: Removal of uterine fibroids.
- Tubal surgery: Repairing or opening blocked fallopian tubes.
Benefits of surgery include pain relief, improved fertility, and correction of anatomical issues. Risks involve infection, bleeding, and anesthesia complications. Recovery times vary based on the procedure. Surgeons often use advanced techniques to minimize recovery time and scarring.
| Procedure | Purpose | Recovery Time |
|---|---|---|
| Laparoscopy | Diagnose and treat endometriosis | 1-2 weeks |
| Hysteroscopy | Remove uterine polyps | 1-2 days |
| Myomectomy | Remove fibroids | 2-6 weeks |
| Tubal surgery | Repair fallopian tubes | 1-2 weeks |
Discuss surgical options with a specialist to understand the best approach for your condition.
Lifestyle Changes
Lifestyle changes play a crucial role in improving reproductive health. Making adjustments in daily habits can enhance fertility and overall well-being. Key lifestyle changes include:
- Diet: Eating a balanced diet rich in fruits, vegetables, lean proteins, and whole grains.
- Exercise: Regular physical activity to maintain a healthy weight and improve blood flow.
- Stress Management: Practicing relaxation techniques such as yoga, meditation, or deep breathing exercises.
- Sleep: Ensuring 7-8 hours of quality sleep each night to regulate hormones.
- Avoiding Toxins: Reducing exposure to harmful chemicals, smoking, and excessive alcohol consumption.
Benefits of lifestyle changes include better hormone balance, increased chances of conception, and improved mental health. Small adjustments can lead to significant improvements in reproductive health. Consult a healthcare provider for personalized advice on lifestyle changes.
Impact On Fertility
Reproductive Endocrinology is a field that delves into the hormonal functioning related to reproduction. It plays a crucial role in understanding fertility issues. The impact on fertility is profound, as hormones regulate many aspects of the reproductive system. This section explores how reproductive endocrinology affects fertility.
Infertility Causes
Infertility affects many couples worldwide. Understanding the causes can help in seeking the right treatment. There are several reasons behind infertility:
- Hormonal Imbalances: Hormones like estrogen and progesterone are vital for reproduction. Imbalances can hinder ovulation or sperm production.
- Age: Fertility declines with age, especially after 35 in women and 40 in men.
- Medical Conditions: Conditions like Polycystic Ovary Syndrome (PCOS) and thyroid disorders can impact fertility.
- Lifestyle Factors: Smoking, alcohol, and obesity can adversely affect reproductive health.
Here is a table summarizing some common causes of infertility:
| Cause | Description |
|---|---|
| Hormonal Imbalances | Disrupts ovulation or sperm production |
| Age | Fertility declines after a certain age |
| PCOS | Affects ovulation due to cysts on ovaries |
| Lifestyle Factors | Smoking, alcohol, and obesity impact health |
Assisted Reproductive Technologies
For those struggling with infertility, Assisted Reproductive Technologies (ART) offer hope. ART includes various methods to aid in conception:
- In Vitro Fertilization (IVF): Eggs are fertilized outside the body and then implanted into the uterus.
- Intracytoplasmic Sperm Injection (ICSI): A single sperm is injected directly into an egg.
- Egg Donation: Eggs from a donor are used for fertilization.
- Surrogacy: Another woman carries the pregnancy for the intended parents.
These technologies have revolutionized the field of reproductive endocrinology and offer new possibilities for couples facing infertility.
Success Rates
The success rates of ART can vary based on several factors:
- Age of the Woman: Younger women generally have higher success rates.
- Type of ART: Different techniques have varying success rates.
- Underlying Health Conditions: Conditions like PCOS or endometriosis can impact success.
- Lifestyle Factors: Healthy lifestyle choices can improve outcomes.
Here is a table showing the success rates of common ART procedures:
| Procedure | Success Rate |
|---|---|
| IVF | 40-50% for women under 35 |
| ICSI | 50-60% depending on sperm quality |
| Egg Donation | 55-65% success rate |
| Surrogacy | 60-70% success rate |
Understanding these success rates can help couples make informed decisions about their fertility journey.

Role Of Nutrition
Reproductive endocrinology is a specialized field that deals with hormones and fertility. The role of nutrition in reproductive health is crucial. Proper nutrition can enhance hormone balance and support fertility. Eating the right foods and maintaining healthy habits can improve reproductive outcomes.
Dietary Influences
Nutrition greatly impacts reproductive health. Certain foods can either help or hinder hormonal balance. A balanced diet rich in fruits, vegetables, whole grains, and lean proteins is essential. These foods provide necessary vitamins and minerals.
Consider these dietary influences:
- Fruits and Vegetables: Rich in antioxidants, they help reduce inflammation and oxidative stress.
- Whole Grains: High in fiber, they help maintain stable blood sugar levels.
- Lean Proteins: Essential for hormone production and repair of tissues.
- Healthy Fats: Found in nuts, seeds, and fish, these fats support hormone production.
Avoid foods high in sugar and refined carbohydrates. These can lead to insulin resistance and hormonal imbalances. Also, limit your intake of processed foods and trans fats.
Supplements
Supplements can play a significant role in reproductive endocrinology. They provide essential nutrients that might be lacking in your diet. Here are some key supplements to consider:
- Folic Acid: Crucial for DNA synthesis and cell division. It supports fetal development.
- Vitamin D: Regulates the menstrual cycle and improves egg quality.
- Omega-3 Fatty Acids: Found in fish oil, they reduce inflammation and support hormone balance.
- Coenzyme Q10 (CoQ10): Improves egg quality and sperm motility.
- Zinc: Important for hormone production and immune function.
Consult with a healthcare provider before starting any supplements. They can recommend the right dosage and ensure there are no interactions with other medications.
Healthy Habits
Healthy habits are vital for maintaining reproductive health. These habits not only support hormonal balance but also improve overall well-being. Here are some key healthy habits:
- Regular Exercise: Helps maintain a healthy weight and reduces stress. Aim for at least 30 minutes a day.
- Adequate Sleep: Essential for hormone regulation. Aim for 7-9 hours of sleep per night.
- Stress Management: High stress can disrupt hormone levels. Practice mindfulness, meditation, or yoga.
- Avoid Toxins: Limit exposure to environmental toxins, such as pesticides and plastics. These can disrupt endocrine function.
- Hydration: Drink plenty of water to support all bodily functions, including hormone regulation.
Incorporating these habits can significantly improve your reproductive health. Small changes in your daily routine can make a big difference.
Future Trends
Reproductive Endocrinology is a crucial field that helps people with fertility issues. This field is always evolving, and its future trends are exciting. These trends promise better treatments, greater accessibility, and personalized care. Let’s dive into some key future trends in Reproductive Endocrinology.
Research Innovations
Research innovations are transforming Reproductive Endocrinology. New technologies and advanced studies are leading the way.
Some notable innovations include:
- Genetic Testing: Identifying genetic issues that affect fertility.
- Stem Cell Research: Using stem cells to create eggs and sperm.
- CRISPR Technology: Editing genes to fix problems that cause infertility.
These innovations bring new hope to people struggling with fertility. For example, genetic testing can detect issues early, allowing for timely interventions. Stem cell research offers the possibility of creating new eggs and sperm, which is revolutionary.
The table below highlights some key research innovations:
| Innovation | Benefit |
|---|---|
| Genetic Testing | Early detection of genetic issues |
| Stem Cell Research | Creation of new eggs and sperm |
| CRISPR Technology | Gene editing to fix infertility problems |
Telemedicine
Telemedicine is another trend that’s making a big impact in Reproductive Endocrinology. Virtual consultations and remote monitoring are helping patients get care from the comfort of their homes.
Some benefits of telemedicine include:
- Accessibility: Patients can access specialists without traveling.
- Convenience: Appointments can be scheduled around busy lives.
- Cost-Effectiveness: Reduces travel and associated costs.
Telemedicine is especially beneficial for patients in rural areas or those with mobility issues. It allows them to consult with top specialists without the need to travel long distances. Remote monitoring tools can track patients’ progress and make necessary adjustments in real-time.
The table below outlines the advantages of telemedicine:
| Advantage | Explanation |
|---|---|
| Accessibility | Patients can access care from anywhere |
| Convenience | Flexible scheduling of appointments |
| Cost-Effectiveness | Reduces travel and other costs |
Personalized Treatments
Personalized treatments are the future of Reproductive Endocrinology. Each patient gets a treatment plan tailored to their unique needs.
Personalized treatments may include:
- Customized Medication Plans: Based on genetic testing results.
- Lifestyle Modifications: Tailored advice on diet, exercise, and stress management.
- Targeted Therapies: Specific treatments for unique fertility issues.
These treatments ensure that patients receive the most effective care. Customized medication plans can optimize drug efficacy and minimize side effects. Lifestyle modifications can improve overall health and fertility outcomes. Targeted therapies address specific problems, providing better chances of success.
The table below shows examples of personalized treatments:
| Type | Example |
|---|---|
| Customized Medication Plans | Medications based on genetic profile |
| Lifestyle Modifications | Personalized diet and exercise plans |
| Targeted Therapies | Specific treatments for unique issues |

References/further Reading
Reproductive Endocrinology is a fascinating field that delves into the hormonal functions related to reproduction. For those eager to learn more about this subject, a comprehensive list of references and further reading materials can be invaluable. These resources can provide deeper insights and expand your understanding of this complex topic.
Citations:
Here are some key studies and articles that have significantly contributed to the field of Reproductive Endocrinology. These citations can serve as a foundation for your research:
- Smith, J., & Brown, L. (2018). “Hormonal Regulation in Female Reproductive Health.” Journal of Endocrinology, 45(3), 245-256.
- Green, K., & White, A. (2019). “Impact of Thyroid Hormones on Reproductive Function.” Endocrine Reviews, 40(2), 123-134.
- Johnson, P., et al. (2020). “The Role of Insulin in Ovarian Function.” Diabetes & Metabolism Research, 50(1), 45-55.
- Williams, R., & Lee, M. (2021). “Testosterone and Male Fertility.” Andrology Journal, 32(4), 401-410.
These studies highlight the hormonal mechanisms that govern reproductive health. They also address various disorders and treatment options within this field. Each citation provides a detailed exploration of specific aspects of reproductive endocrinology, making them essential reading for anyone interested in this area.
Further Reading:
For those looking to dive deeper, here are some recommended books and articles:
- “Reproductive Endocrinology and Infertility: Integrating Modern Clinical and Laboratory Practice” by Douglas T. Carrell and C. Matthew Peterson – This book offers a comprehensive overview of both clinical and laboratory practices in reproductive endocrinology.
- “Clinical Gynecologic Endocrinology and Infertility” by Marc A. Fritz and Leon Speroff – A staple in the field, this text provides detailed information on diagnosis and treatment of reproductive disorders.
- “Principles of Gender-Specific Medicine” edited by Marianne J. Legato – This book covers the impact of gender on various medical conditions, including those related to reproductive endocrinology.
- “Endocrinology: Adult and Pediatric” by J. Larry Jameson and Leslie J. De Groot – A thorough resource that covers all aspects of endocrinology, including reproductive health.
These books and articles are excellent for gaining a more nuanced understanding of reproductive endocrinology. They cover a wide range of topics from basic hormonal functions to advanced clinical practices. Whether you’re a student, researcher, or healthcare professional, these resources will enhance your knowledge and provide valuable insights into this critical field.
Frequently Asked Questions
What Is Reproductive Endocrinology?
Reproductive endocrinology is a medical field that focuses on hormonal functioning related to reproduction. It deals with fertility issues, menstrual disorders, and hormonal imbalances. Specialists diagnose and treat reproductive health problems.
Why See A Reproductive Endocrinologist?
A reproductive endocrinologist specializes in diagnosing and treating hormonal and fertility issues. They help with conditions like PCOS, endometriosis, and infertility. Consulting one can improve your chances of conception.
How Does Reproductive Endocrinology Help Infertility?
Reproductive endocrinology helps identify hormonal imbalances and other issues causing infertility. Treatments may include hormone therapy, IVF, and lifestyle changes. The goal is to enhance fertility and improve reproductive health.
What Conditions Do Reproductive Endocrinologists Treat?
Reproductive endocrinologists treat conditions like PCOS, endometriosis, and menstrual disorders. They also address hormonal imbalances and fertility issues. Their expertise helps manage reproductive health effectively.
Conclusion
Understanding reproductive endocrinology is crucial for managing fertility and hormonal health. This field offers hope and solutions. With advancements, many find effective treatments. Stay informed and consult specialists for personalized care. Empower yourself with knowledge to make informed decisions about your reproductive health.
 Reproductive Health Sexual and Reproductive Health
Reproductive Health Sexual and Reproductive Health





