 Decoding Male Anatomy: The Complete Guide to Labeled Seminal Gland Models
Decoding Male Anatomy: The Complete Guide to Labeled Seminal Gland Models
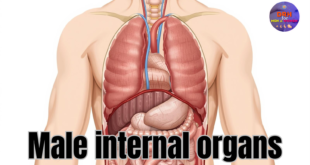
The male reproductive system is a marvel of biological engineering, yet it remains a subject that many students and even some healthcare professionals find challenging to visualize in three dimensions. Among the various components, the seminal glands (also known as seminal vesicles) play a critical role that is often overshadowed by more prominent organs like the prostate or testes. However, understanding the precise anatomy of these glands is vital for urology, reproductive medicine, and general anatomy education.
Textbooks provide a solid foundation, but 2D diagrams often fail to convey the complex, tortuous structure of these glands or their spatial relationship with the bladder and rectum. This is where anatomical models bridge the gap. A high-quality, labeled seminal gland model transforms abstract medical concepts into tangible, visual realities. By breaking down the specific components of these models, we can gain a deeper appreciation for how male physiology functions and how medical professionals diagnose and treat related conditions.
What Are Seminal Gland Models?
Seminal gland models are three-dimensional representations of the male internal reproductive organs, specifically focusing on the seminal vesicles and their immediate anatomical neighbors. These tools range from simple, schematic plastic casts designed for high school biology classes to highly intricate, medically accurate reproductions used in surgical planning and advanced medical training.
The primary purpose of these models is to offer a spatial perspective that flat images cannot. In a typical model, you will see the paired seminal glands situated behind the bladder and above the prostate. Labeled versions are particularly valuable because they identify specific landmarks—ducts, lobes, and vascular connections—allowing learners to trace the path of reproductive fluids physically. They serve as essential bridge tools, helping students move from memorizing terms to understanding physiological systems.
Anatomy Breakdown: The Labeled Seminal Gland Model
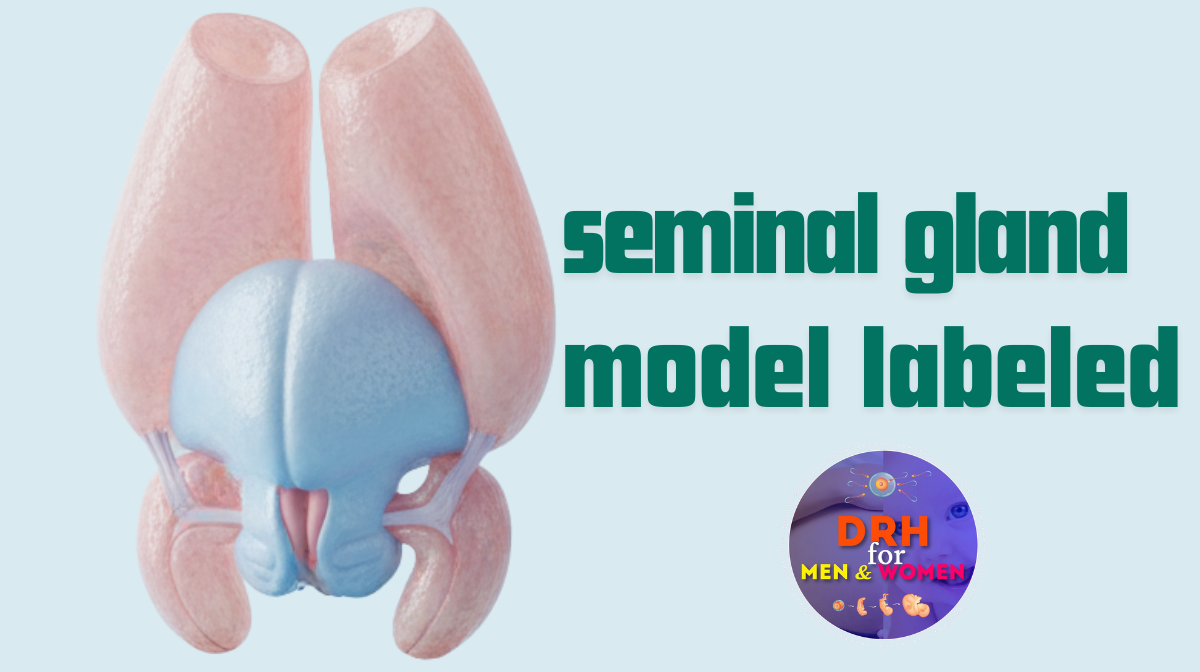
When you look at a professional-grade labeled seminal gland model, you aren’t just looking at a generic lump of tissue. You are looking at a highly specific map of the reproductive infrastructure. Here is a detailed breakdown of the parts typically identified on these models and their physiological functions.
The Seminal Vesicle Body
The most prominent feature of the model is the body of the gland itself. On a detailed model, this appears not as a smooth sac, but as a coiled, convoluted tube. If unraveled, this tube would be significantly longer, but nature has packed it efficiently to fit within the pelvic cavity.
- Function: This is the factory floor. The epithelial lining here secretes a thick, alkaline fluid rich in fructose (sugar), prostaglandins, and clotting proteins. This fluid makes up about 60-70% of the total semen volume and provides the energy sperm need to swim.
The Excretory Duct
At the base of the seminal vesicle, the model will show the structure narrowing significantly. This creates a funnel-like exit known as the excretory duct.
- Function: This duct acts as the drainpipe for the fluid produced in the main body, guiding it toward the urethra.
The Ampulla of the Vas Deferens
While not part of the gland itself, the vas deferens is almost always included in these models because of its critical connection. The “ampulla” is the enlarged, reservoir-like section of the vas deferens seen right next to the seminal vesicle.
- Function: This area stores mature sperm before ejaculation. On the model, seeing the ampulla next to the seminal vesicle helps students understand how sperm and seminal fluid meet.
The Ejaculatory Duct
This is perhaps the most critical junction point on the model. It is formed where the excretory duct of the seminal gland merges with the vas deferens.
- Function: This duct passes through the prostate gland and empties into the urethra. It is the mixing chamber where sperm and seminal fluid combine before being propelled out of the body.
The Prostate Gland (Posterior View)
Most seminal gland models provide context by including the posterior surface of the prostate. The seminal glands sit superior to (above) the prostate.
- Function: Understanding this relationship is crucial for diagnosing conditions like Benign Prostatic Hyperplasia (BPH) or prostate cancer, which can impinge on the seminal vesicles or ejaculatory ducts.
A Brief History of Anatomical Modeling
The use of models to study the human body has a rich history. Long before plastic injection molding, Renaissance anatomists used wax to create incredibly lifelike representations of internal organs. The famous “La Specola” collection in Florence dates back to the late 18th century and includes wax models of the male reproductive system that are still anatomically relevant today.
For the seminal glands specifically, early models were often crude, depicting them as simple sacs. It wasn’t until corrosion casting techniques became popular—where resin is injected into ducts and the tissue dissolved away—that anatomists fully understood the complex, singular tubular nature of the vesicle.
Today, the evolution continues with 3D printing. We have moved from generalized “average” models to patient-specific models printed from MRI or CT scan data. This allows a surgeon to hold a model of a specific patient’s anatomy before ever making an incision.
Step-by-Step Guide to Using a Labeled Model
Owning a model is one thing; using it effectively for study is another. Here is a systematic approach to getting the most out of a labeled seminal gland model.
1. Orient the Anatomy
Start by establishing direction. Locate the bladder (usually the smooth, large round structure) and the prostate (the walnut-sized gland at the base). Identify the posterior (back) view, as the seminal vesicles are best viewed from behind the bladder.
2. Trace the Fluid Pathway
Use your finger or a pointer to trace the “journey.” Start at the ampulla of the vas deferens (sperm arrival) and the body of the seminal vesicle (fluid production). Follow both down to where they merge at the ejaculatory duct. This kinetic tracing reinforces the physiological sequence of ejaculation.
3. Cross-Reference with Cross-Sections
Many high-end models come with a cross-section view. Compare the external coiled appearance with the internal honeycomb structure shown in the cross-section. This helps in understanding the massive surface area available for fluid secretion.
4. The “Blind” Test
Once you are familiar with the structures, cover the labels or key card. Point to a structure, name it, and explain its function aloud. Active recall is significantly more effective than passive observation.
Why Use Models? The Benefits for Research and Education
In an era of high-definition digital rendering, one might ask if physical models are still necessary. The answer is a resounding yes.
Tactile Learning: Humans are tactile creatures. Being able to rotate a model, feel the difference in texture between the muscular vas deferens and the glandular seminal vesicle, and see the depth of the structures creates a stronger memory anchor than a screen ever could.
Spatial Awareness: It is notoriously difficult to understand the angle of the ejaculatory duct as it enters the prostate using only 2D images. A physical model clarifies these 3D relationships instantly, which is vital for surgical students learning to avoid accidental injury during pelvic surgeries.
Patient Communication: For doctors, models are empathy tools. When a patient is diagnosed with a blockage or a cyst in the reproductive tract, showing them a model demystifies the condition. It turns a scary, abstract diagnosis into a mechanical issue that can be visualized and understood.
Real-World Applications
Seminal gland models are utilized across various sectors of medicine and science.
Medical Training and Surgery
In medical school, these models are staples in gross anatomy labs. For urology residents, advanced models are used to practice transrectal ultrasound (TRUS) interpretations. By comparing the ultrasound image to the physical model, residents learn to identify the “bowtie” appearance of the seminal vesicles on a scan.
Fertility Clinics
In fertility medicine, these models help explain causes of male infertility. For example, if a patient has a blockage in the ejaculatory duct, a specialist can use the model to show exactly where the blockage is preventing sperm from mixing with seminal fluid, explaining why the patient has low semen volume (aspermia) or no sperm (azoospermia).
Pathological Research
Researchers studying prostate cancer often use models to map how tumors spread. Because the seminal vesicles are attached to the prostate, they are a common route for cancer invasion. Models help researchers visualize tumor staging (e.g., Stage T3b prostate cancer involves invasion of the seminal vesicles).
Challenges and Limitations
Despite their utility, models are not perfect. A significant challenge is anatomical variation. A standard labeled model represents the “textbook” male. In reality, seminal vesicles vary wildly in size, symmetry, and shape between individuals. Relying solely on a model can lead students to expect a uniformity that does not exist in clinical practice.
Furthermore, most models are static. They are rigid plastic or resin. They cannot demonstrate the dynamic contraction of the muscular wall during ejaculation or the physiological changes that occur with age or disease. While some high-fidelity silicone models attempt to mimic tissue texture, they still lack the dynamic blood flow and nerve response of living tissue.
Future Trends in Anatomical Modeling
The future of seminal gland modeling is hybrid and hyper-realistic. We are seeing a shift toward:
- Augmented Reality (AR) Overlays: Students wearing AR glasses can look at a physical model and see a digital overlay of blood flow, nerve impulses, or lymphatic drainage mapped directly onto the plastic structure.
- 3D Bioprinting: Research is moving toward printing models using biological materials that react like real tissue. This would allow surgeons to practice cutting and suturing on a material that behaves exactly like a human seminal vesicle.
- Haptic Feedback: Digital models are incorporating haptic technology, allowing users to “feel” the resistance of tissue through a stylus, simulating the sensation of performing a biopsy or injection.
Expert Insights
Urologists and anatomy professors consistently advocate for the integration of physical models in early education. Dr. James H., a senior lecturer in clinical anatomy, notes that examination scores regarding pelvic anatomy often improve when students have access to manipulatable models rather than just dissection software.
Similarly, patient advocacy groups highlight that patient compliance improves when physicians use visual aids. When a man understands the mechanics of his condition via a clear, labeled model, he is more likely to follow through with treatment plans or necessary lifestyle changes.
Conclusion
The labeled seminal gland model is more than just a piece of plastic in a doctor’s office. It is an educational cornerstone that bridges the gap between confusing diagrams and the complex reality of human biology. From the coiled body of the vesicle to the crucial junction of the ejaculatory duct, these models provide the spatial context necessary for true understanding.
Whether you are a medical student trying to pass an anatomy exam, a researcher investigating reproductive pathology, or a patient seeking to understand your own body, these models offer clarity. As technology advances, the fidelity of these tools will only improve, but the fundamental value of seeing and touching the anatomy remains unchanged.
Q&A Section
Q: Is the seminal gland the same thing as the seminal vesicle?
A: Yes, the terms are used interchangeably. “Seminal vesicle” is the older, more common term, while “seminal gland” is often preferred in modern anatomical terminology because the structure is glandular (secreting fluid) rather than just a vesicle (sac).
Q: Can you feel the seminal glands during a physical exam?
A: Generally, healthy seminal vesicles are soft and difficult to palpate during a digital rectal exam (DRE). However, if they are inflamed, enlarged, or hardened by disease, a physician may be able to feel them above the prostate.
Q: What happens if the seminal glands are removed?
A: Removal (vesiculectomy) is rare but can occur during radical prostatectomy for cancer. Without them, a man cannot ejaculate normal semen volume, rendering him infertile naturally, though sperm is still produced in the testes.
Q: Why do the seminal glands look like honeycomb inside?
A: The interior is made of many folds and pockets (mucosal folds). This maximizes the surface area, allowing for greater production and storage of the fructose-rich fluid essential for sperm survival.
Resources
For those looking to purchase models or further their study, the following resources are valuable:
- Anatomy Stuff & 3B Scientific: Leading suppliers of medical-grade anatomical models.
- Radiopaedia: An excellent digital resource for viewing seminal glands in MRI and CT scans to compare with physical models.
- The Visible Human Project: Provides detailed cross-sectional images of the human body for digital reference.
 Reproductive Health Sexual and Reproductive Health
Reproductive Health Sexual and Reproductive Health